Breast implant removal (also called breast explant surgery) may be considered for a variety of reasons.
Here are some common issues presented by Dr. Rudderman’s patients:
- “ I no longer feel my breast implants fit my lifestyle and desires.”
- “ My breast shape and feel has changed, and one side is too firm.”
- “ I am concerned that having implants may be impacting my health”
- “ I’m no longer comfortable with the size of my breast.”
- “ I may have a ruptured my breast implant, and am concerned that a leak may occur.”
- “ I’ve gained weight, and my breast are now too large.”
Why Do Women Consider Breast Implant Removal?
- Some women who had breast augmentations find after maturing and lifestyle changes (such as pregnancy or weight gain/loss) that their breasts are now larger or different shape than desired.
- Breast size may have increased during menopause.
- Breast may feel too large and uncomfortable and are no longer consistent with their style preference.
- Many women are concerned about postponing breast implant removal or explant surgery and being older with thinner skin and perhaps less stamina for surgery.
- Some women are concerned that their implants may be impacting their health.
- Some women feel that they were never particularly happy with the decision for augmentation in the first place.
What Are The Most Common Breast Implant Removal Concerns?
Here are some common patient concerns when breast implants are removed:
- “Will I look deflated?”
- “Will my clothing fit”
- “How will I feel about my breast change”
- “How will my partner feel about my breast change”
- “Will I need additional surgery to address drooping or sagging or uneven breasts and can this be safely and reliably done.”
Dr. Rudderman has treated hundreds of women with breast implants placed at one time in their life who have decided to return to a more natural state. While breast implants may last for decades, the reality is that anyone who has breast implants at some point should expect to need implant removal, replacement, or revision. Implants are not considered lifetime devices.
Will a Breast Lift or Mastopexy Improve My Appearance When my Breast Implants are Removed?
Many patients have adequate breast volume to have a normal appearance after implant removal. Some find that their breast volume has increased over time, particularly with weight changes, pregnancy, and menopause. A breast lift can help reshape and restore a more youthful breast look and can be associated with dramatic improvement in comfort.
Some women avoid having a breast lift after implant removal due to concerns about scarring and healing. It is not uncommon for a surgeon to advise you to keep your implants or have new breast implants inserted. Many women simply no longer want this option.
Patients who undergo Dr Rudderman’s detailed implant removal and lift technique are often extremely pleased with their appearance for the first time in years.
What Determines if I’m a Good Candidate for Breast Implant Removal?
During the consultation, your breast will be examined to determine your natural breast and soft tissue covering, implant positioning, size, and condition. Probable volume and contour changes anticipated after removing implants will be estimated and reviewed, as will the potential need for a combined surgical procedures like a lift or reshaping, or option for future breast lift if needed and desired.
Many patients do well with implant removal and lift without future surgery required.
What Are The Most Common Reasons for Considering Breast Implant Removal?
- Change in breast shape
- Hardening of the breast (capsular contracture)
- Ruptured or leaking breast implants
- Concern for health impact with implants (breast implant illness)
- No longer enjoy the look or feel of the breast
- Want to return to a natural state that won’t require more surgery in the future
Before and After Photos
A gallery of images to assist in finding the sample results you might be looking for in surgical, injectables, and med spa.
Change in Breast Shape
Breast implant removal can be considered when your breast shape changes over time and you feel your breasts are unattractive or uncomfortable.
Women with implants often see breast changes as they age due to:
- weight fluctuations
- pregnancy that results in asymmetry
- misshapen breasts
- breasts that appear unbalanced
- well-placed implants that cause discomfort or visual concern over time
Many women feel their breast implants were always too large or noticed an unpleasant shape after surgery. Often removal of breast implants may result in a more natural-looking breast.
During the consultation, we will examine your breast and implant position size, tissue characteristics, and volume and contour changes anticipated following removal of your implants. A breast lift may be a good option at the time of removal or in the future if desired.
Hardening of the Breasts (Capsular Contraction)
A known complication of breast implant placement is the occurrence of capsular contraction. All breast implants placed in the body become surrounded by a layer of tissue called a capsule that in most patients stays soft and thin. This is the body’s natural response to an implant. However, some women will find that one or both breasts may become firm or hard overtime resulting breast change and shape. This hardness can be noticeable over weeks or may be so gradual that they may not be able to remember when their breast first became firm, hard, or misshapen.
Capsular contraction is believed in some cases to occur because of a reaction to the natural bacteria within the breast tissue that stimulate a response causing the capsule tissue to contract. These are not considered infections and treatment with antibiotics does not result in resolution. Capsular contraction is also often associated with ruptured implants, particularly when significant chronic inflammatory changes occur. Capsules, when tightened, may become thickened or remain thin and still cause implant shape change. Capsular contraction can occur with saline or silicone implants, textured or smooth implants, and with implants placed above or below the muscle.
Many patients will complain of:
- Pain
- Discomfort
- Soreness
- Shape change
- Interference with physical or sexual activity
The capsule can adhere to the surrounding muscle and breast tissue and can cause interference during physical activity and movement and result in muscle and nerve inflammation.
Patients may experience discomfort in the chest, shoulder, rib, and back, numbness, tightness, heaviness, or nonspecific irritation from capsular contractures. Some will be embarrassed to give someone a hug because their breasts just feel “rock hard”.
Encapsulated Breast Implant
- Breast Implant Age: 28 years
- Breast Implant Type: Saline
- Breast Implant Size: Unknown
- Breast Implant Placement: Subglandular
- Reason for Explant Surgery: Breast implant age, bilateral hardening of breasts, pain, and discomfort
- Surgery Performed: Bilateral breast implant removal and bilateral capsulectomy, enbloc

Treatment Options for Capsular Contraction
Many women decide to have implants removed after developing a capsular contraction. If replacement of the implants is considered, brand new implants should be used, and the capsules removed in most cases. Using the original implants is not recommended due to the possibility that the implant surface has adherent bacteria called a biofilm. And you may be at greater risk for a recurrence of the contracture after surgery.
In most cases, a capsulectomy (the surgical removal of the capsule) is performed at the time of implant replacement to potentially reduce the recurrence rate of the capsular contraction. Removal of the capsule generally results in a dramatic breast shape change. Surgery, however, does not ensure that a capsular contraction will not recur and patients who have had a previous contraction may be at significantly higher risk of subsequent capsular contractions. Capsule removal may as well result in more lateral positioning of any replaced breast implant due to pocket size change.
During your consultation, Dr. Rudderman will assess implant positioning, size, capsular contracture severity, and soft tissue characteristics. Many symptoms associated with the mechanical effects of a capsule, restricting movement, adherence to surrounding tissues, may resolve quickly after implant and capsule removal.
Ruptured or Leaking Breast Implants
Breast implant should be removed when evidence of rupture or leak is encountered. A routine mammogram may reveal an implant rupture. MRI or ultrasound test may also show a rupture or leak. A ruptured implant is considered a mechanical failure of the implant with a break in the silicone lining of the implant.
When the breast implants are saline, the breast will often become much smaller within one to several days as the saline is absorbed by the surrounding tissue. Many women will experience some soreness or discomfort from mild inflammation caused by this process. In the past, some surgeons were known to add antibiotics or soap solutions such as Betadine to the saline implants when filled, these patients may experience more inflammation following rupture.
When the implants are silicone gel-filled, any rupture of the implant may allow the gel to leak into the capsule. Older implants were constructed with less cohesive (sticky) gel that acted more like a thick sticky liquid. The most recent implants are made using cohesive gel technology that helps restrict leakage even with implant rupture. Current data has demonstrated silicone material in the capsules of patients with gel implants even without rupture. Silicone has not been documented in capsules surrounding saline implants.
Implants in some cases may be ruptured for years before a patient experiences any shape changes and, in some women, a ruptured implant may not result in a dramatic shape change.
Some women will develop significant inflammation following implant rupture. This will often result in the thickening of the capsule around the implant and in many women long term ruptures may result in calcification of the capsule. Calcification results in changes of the visible lining of the capsule where calcified areas may resemble eggshell fragments. These changes are always associated with some inflammation of the surrounding capsular tissue. When implants are removed for any reason and calcification is encountered, a capsulectomy is performed (surgical removal of the capsule), and the capsules are sent for pathologic evaluation. These patients typically receive a written report of findings from the pathologist.
Concerns for General Health
Many women desire to have implant removal due to their concern that the implants are impacting their general health. Many U.S. & International studies indicate the difficulty in specifically relating implants to specific medical conditions. None the less, many women feel they do not do well with breast implants.
Some women will voice concern of general medical and health changes within a year having breast implant surgery. Many will present years later with concerns regarding breast implants and general health.
Some women may have localized breast or chest wall discomfort and visible changes. Other will have no visible breast changes or local pain or discomfort and may have a normal breast exam and still experience health issues. Patients may notice a gradual onset of new symptoms relating to a specific condition or may just generally not feeling well.
Multiple studies have been done supported by the American Society of Plastic Surgeons to determine relationship of symptoms to breast implants. Factors evaluated include material reactions, heavy metals, allergy, inflammatory changes, infections, biofilms, and autoimmune complexes, and recovery or reduction of symptoms following surgery. To date, no direct link has been established. However symptom reduction is statistically very significant with implant removal independent of capsule treatment in these studies.
Women who visit our office for breast implant evaluation are often sent by their general practitioner, rheumatologist, health consultant, or concerned friend. Some women have been evaluated by other surgeons who may either dismiss their symptoms of concern or recommend extreme solutions for treatment.
It is not possible to accurately predict if an implant removal patient experiencing medical problems will see a positive impact on their health. However, many women will report significant and often dramatic improvement in concerns soon after implant removal.
Symptoms can range from general fatigue to significant disability.
Some of the most common complaints are:
- Extreme fatigue that simply does not resolve with “adequate” rest
- Women that have a history of enjoying being physically active find that instead of being energized after exercise, more rest is required
- Hair loss
- Cardiac concerns often culminating in cardiac workup in younger patients with no contributing factors. Often these patients end up having full cardiac workups that are negative.
- Allergies
- Digestive issues – variable food and substance sensitivities. These patients often report GI evaluation, often upper and lower GI scoping with no specific findings and no resolution of symptoms.
- Skin changes and rashes that don’t seem to respond to treatment even with the best dermatologic evaluation
- Joint pains that seem to migrate, and are in distributions not common with rheumatoid disease, osteoarthritis, or fibromyalgia, and not responsive to traditionally effective medications.
- Sleep disturbance, anxiety, in women with no prior history, not responsive to traditional medical treatments.
- Depression
- A wide range of other symptoms have been reported as well
- Endocrine disruption, often requiring supplemental treatments including Thyroid replacement.
- and a wide variety of issues often seen in autoimmune complexes
Many of Dr. Ruderman’s patients describe a similar story; they have been to their family practice doctor, and/or gynecologist who could find no objective lab evidence for their health concerns. Many patients have spent additional time and resources on more extensive labs, tests, x-rays, scans, all without a diagnosis. This leads to frustration, unresolved concern, and in some cases depression.
Dr. Rudderman understands the decision to remove implants is not an easy decision. It can be agonizing to trade aesthetic concerns for the uncertainty of “if I will feel better”. However, many women (88%) often report improvement or resolution of specific complaints very soon after implant removal.
Current data published from the ASPS supports the % improvement in symptoms. These studies do not confirm association linked to infection, allergy, material toxicity, autoimmune reaction, inflammatory syndromes.
Patients do specifically report seeing rashes resolve, hair growth resume, allergies subside, pain resolve, typically beyond what would be expected by nocebo alone. There are some who report such significant improvement that they can reduce or eliminate medications they have been taking for years to treat their symptoms.
Surgical Options for Breast Implant Removal
Women who present for implant removal evaluation, in many cases, have health concerns. The general expectation for treatment includes implant removal and capsulectomy. The capsule is the tissue that your body makes that surrounds the implant. This is the “normal” reaction to foreign objects placed in the body. This tissue is living tissue with a vascular supply (blood supply). Dr. Rudderman does not recommend additional operations such as lymph node removal. A lymph node removal operation carries additional long term and significant risk and is not considered appropriate unless other health concerns are documented. Limiting surgery to the safest and least invasive method is often the best way to help restore prior breast health.
Modified “En Bloc” Implant Removal (Total Capsulectomy with Implant Removal)
True enbloc resections “require” as described removal without creating any opening in the capsule and it is a term reserved for “tumor” resection. This approach by description is associated with additional known risk, and has not demonstrated greater reduction in post-operative symptoms in current studies. This technique that involves removing the implant with the surrounding lining as a single unit is more accurately described as a total intact capsulectomy. In order to successfully achieve this result a significantly larger incision is required. Patients must realize when implants are first put in place, the incisions may be quite short -often 4 cm or less. However, removal of an implant cannot be done through the same incision size and if an intact total capsulectomy resection is to be performed, the incisions can be as long as 8-14 – cm or more. And large incisions alone do not guarantee in any way that this operation can be performed. The incision is usually in the inframammary crease – the fold under the breast – and may include the original incision if the implant was placed through the site.
Implants placed above the muscle may be most successfully removed with capsule intact. Implants placed below the muscle may be removed with this outcome if the capsules are significantly thick enough to allow for dissection without disturbing surrounding normal tissue. Implant capsules behind the implant and adjacent to the ribs may be too thin to perform this type of resection due to risk of damage to ribs, lung, and cardiac space and muscle depending upon conditions found during the actual surgery. Some women may be a candidate for this implant capsule removal technique depending on intraoperative findings.
The potential advantage of removal of the capsule intact is that it may help control the removal of ruptured gel and calcified tissue, potential biofilm from bacteria, and other inflammatory components during implant and capsule removal. There are specifically increased risks associated with capsulectomy approaches of all techniques particularly with thin capsules.
The end result however is a capsulectomy (removal of all safely resect able capsular tissue). Studies indicate that patients treated with this approach report a greater than 88% chance of resolution of some concerning symptoms. Removing the implant and leaving the capsule may eventually result in the capsule resorbing, and has been used as an option for treatment based on other study results and surgeon recommendations. Current data supports this as an effective option with implant removal. Implant removal surgery performed with any approach to the capsule, thick and calcified, or millimeter thin, should be approached to preserve and protect surrounding normal muscle, bone, cartilage, and soft tissue.
Total Intact Capsulectomy & Breast Implant Removal
- Reason: Breast Implant Capsulectomy
- Patient Age: 55 years old
- Breast Implant Size: 300CC
- Breast Implant Age: 20 years
- Breast Implant Type: Textured Silicone
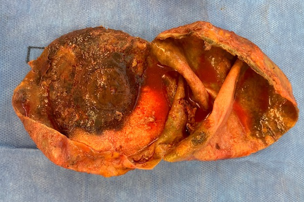
A consultation is required to evaluate your potential for performing and block resection. It is not accurate to state that all implants can be removed safely by “en bloc” resection and the pros and cons should be seriously reviewed during your exam to determine realistic options and expectations.
Consensus Statement on Breast Implant Capsulectomy Definitions and Management Created by Breast Surgery Collaborative Community, The Aesthetic Society/ The Aesthetic Foundation , June 8, 2024
“The FDA recently created a strategic priority for the creation of collaborative communities to bring together stakeholders in the medical device realm to solve challenges and achieve a collective betterment for patients, physicians, industry, as well as the medical community at large. The Breast Surgery Collaborative Community (BSCC), a consortium of patient advocates, board-certified plastic surgeons, the medical device industry, and others with a vested interest in enhancing breast surgery safety, was assembled to offer clarity for women seeking guidance on removal of breast implants related to health concerns. “
“The BSCC consensus statement defines four types of capsulectomy: “
- “Total intact capsulectomy: Complete removal of the breast implant capsule as a single unit.
- Total capsulectomy (total precise capsulectomy): Complete removal of the breast implant capsule, not necessarily done as a single unit or in one piece.
- Partial capsulectomy: Removal of the breast implant capsule where some capsule is left behind.
- En bloc capsulectomy: Removal of the breast implant capsule with a margin of uninvolved tissue for treatment of suspected or established breast implant-associated cancers after appropriate medical workup. “
The statement explicitly declares, “the absolute and only indication for an en bloc capsulectomy is for an established or suspected breast implant-associated cancer after appropriate medical workup.” This decision for surgery is clearly a part of the informed consent process, and any decisions should be shared between the patient and surgeon in a formal discussion around risk assessment, benefits, and alternatives, as well as the expected outcomes. ” The Aesthetic Society June 8, 2024.
Mastopexy After Removal of Implants
During your consultation, Dr. Rudderman will address post implant removal extra skin, soft tissue and adjustments to breast tissue.
Breasts often become more droopy after removing implants. These patients will benefit from a breast lift (mastopexy).
Larger breasts often become more droopy after removing implants. These clients benefit from a breast lift (mastopexy).
Breast lifts work well for women with little breast volume who have concern they may be “traumatized” by the thought of removing implants when they feel the “only” breast tissue they have are the implants. A breast lift in these cases can effectively reduce the skin laxity to “repackage” the remaining breast tissue optimizing the volume in a “smaller” package to improve appearance. The remaining volume of breast can usually be reasonably estimated. There may be areas of asymmetry, wrinkling, or indentations after implant removal that cause concern. Many times these irregularities improve during healing. In the few patients who require additional treatment, additional skin may be removed, tissue repositioned, and in some cases, fat grafting to address contour irregularities.
Dr. Rudderman has successfully performed hundreds of mastopexy operations for breast implant removal patients with great success. Many patients are thrilled with their new breasts post implant removal and are relieved they have achieved satisfying results without implants. Dr. Rudderman’s mastopexy technique may be an excellent solution for patients who no longer desire breast implants and are dedicated to their long term health and well-being.
Fat Grafting
Fat grafting can be effective in select patients that have dimpling, residual asymmetry, and need for “modest” volume. Fat grafting should be performed by a Board-Certified Surgeon with years of experience and for specific indications. There are very well-defined limitations with fat grafting, particularly long-term expectations.
Contact us at 678.566.7200 to meet with Dr. Rudderman in our Alpharetta office or Midtown Atlanta office.
Real Patient Reviews
Written and reviewed by:
Dr. Randy Rudderman, who is board certified by the American Board of Plastic and Reconstructive Surgery (1994). He practices medicine at his offices in Alpharetta and Atlanta. The content written reflects current accurate information and is consistent with ethical positioning of the ASPS. (American Society of Plastic Surgeons).
Last modified: February 2, 2024
Learn more about Dr. Rudderman, his medical training, and credentials.
Should I Remove My Breast Implants?
Some decisions may seem obvious if you experience:
- Hard breasts
- Breast pain or discomfort with exercise
- Unexplained health issues
- Droop
- Feeling that “my breast are under my arms or end up under my armpits when reclining”
- Capsular contractions that recur
- Asymmetry
- Excessive size for comfort physically or psychologically
- Simply “tired of having breast implants”
There are millions of women that love their breast implants, have no symptoms of concern, and no issues with health. Then there are those who have what they describe as “great looking and feeling breast” with implants but have unexplained health concerns, some so severe that now daily life is affected.
These are the difficult decisions, requiring long and thoughtful consultations, and careful deliberation and reflection before selecting surgery as an option. Managing risk and expectations can be effectively and safely done with good patient communication and excellent staff and facility options. Being nervous before surgery is expected, being anxious that you have not made the best choice of surgery or surgeon means you need more time, better education, and a clearer path to health.
Dr. Rudderman has a 25-year track record of successful breast revision surgeries and satisfied patients. Dr. Rudderman is empathic to the very real concerns his patients have about their breast implants.
Breast Implant Removal Frequently Asked Questions
Search our list of FAQs for the answers you are looking for.



